Come on, we have an IUT case!!!

Immunohematology Made Easy (2)
General Topics – Key Principles and Everyday Practices
📘 Available now in PDF & EPUB formats
🔗 Visit Store
Come on, we have an IUT case!!!
In one of the blood banks, this conversation took place between:

Immunohematology Made Easy (2)
General Topics – Key Principles and Everyday Practices
📘 Available now in PDF & EPUB formats
🔗 Visit Store
‘S’ – someone who has been working in the blood bank for a while.
‘T’ – someone who just started working in the blood bank.
S: Ready, dear? Come on, we have an IUT case!
T: IUT? What does that mean? I’ve never heard of that before.
S: Alright, let’s break it down step by step. IUT stands for Intrauterine Transfusion, which is the process of transfusing blood to the fetus.
T: Fetus? You mean the baby after birth, right?
S: No, just as you heard—it’s a blood transfusion to the fetus itself while still inside the womb.
T: That’s very strange! Why would a fetus even need a blood transfusion?
S: The most common reason is severe fetal anemia, which usually happens due to HDFN. Do you remember what HDFN stands for? We talked about it before.
T: Yes! It stands for Hemolytic Disease of the Fetus and Newborn.
S: Exactly! Well done! You just said hemolytic disease of whom? The fetus! So it’s not just about newborns, right?
T: Right, right! Got it.
S: Maternal antibodies cross the placenta and attack antigens on the fetal red blood cells, binding to them and leading to hemolysis.
T: Okay, but something is confusing me—how do they even know the fetus has anemia? They can’t just draw blood from its arm and run a CBC, right?!!!
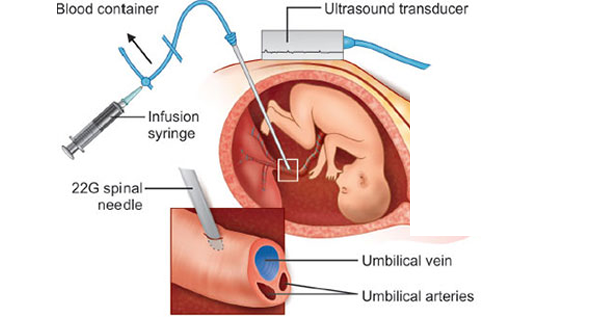
S: Hahaha, of course not! Fetal anemia is mainly diagnosed using Doppler ultrasound, which measures blood flow in a fetal artery called the middle cerebral artery (MCA). Since anemic blood is “lighter,” it moves faster. By comparing the blood flow velocity to gestational age, they can determine whether the anemia is mild or severe. If there is a high suspicion, they can take an additional confirmatory step by performing cordocentesis, which involves drawing a direct blood sample from the fetal umbilical cord.
T: So, if the Doppler confirms anemia, what happens next?
S: At that point, IUT is usually necessary. The goal is to treat the anemia and prevent serious complications for the fetus.
T: Got it! So, how is IUT performed?
S: The procedure is done under sterile conditions, guided by ultrasound. A needle is inserted through the mother’s abdomen into the umbilical vein, and compatible red blood cells are transfused directly into the fetal circulation. This is the most common method of performing the procedure.
T: How much blood is transfused?
S: The volume depends on multiple factors, such as fetal weight and anemia severity. There’s a well-known formula:
Blood Volume Needed=Fetal Weight (g)×0.14×(Desired Hct−Pre-transfusion Hct)/RBC Unit Hct
Let’s break it down:
Fetal Weight (g): Obtained from ultrasound.
0.14 mL/g: An estimated value representing fetal blood volume per gram of fetal weight.
Desired Hematocrit (Hct): The target post-transfusion hematocrit, usually 40-50%.
Fetal Hematocrit (Hct): The current hematocrit level before transfusion.
Hematocrit of Donor Blood: Usually 70-85%.
For example, if:
The fetus weighs 1000 g
The desired hematocrit is 40%
The pre-transfusion hematocrit is 15%
The donor unit hematocrit is 85%
Then:
Blood Volume Needed=1000×0.14×(0.4−0.15)/0.85=41.2 mL
T: Great! Now, what about the blood itself? What are the requirements?
S: The requirements we follow might differ slightly from those of some of our colleagues in other places, as they adhere to their institution’s standards.
For the mother’s sample:
Determine blood type.
Perform antibody screening.
If positive, do antibody identification to determine which antibody is present (since it’s likely causing HDFN).
The transfused unit must be negative for the antigen targeted by the maternal antibody.
If the mother has a previously recorded antibody, we check if any new ones have developed.
For the red blood cell (RBC) unit:
Blood type: O-negative.
Must be compatible with the mother and antigen-negative for any maternal antibodies.
Washed .
Leukoreduced .
Irradiated .
CMV-negative.
Hemoglobin S-negative.
Fresh unit (preferably 5-7 days old).
Hematocrit: 70-85%.
Anticoagulant preservative solutions: Preferably CPDA-1 (or SAGM if washing is available).
T: So, we need a meticulously prepared RBC unit—it’s not just any random unit!
S: Exactly! This is extremely important, and these blood unit specifications are critical for the procedure. We need to work quickly, efficiently, and with absolute precision.
T: Thank you so much! I’ve really learned a lot today.
S: No problem, dear! May we always be a source of help and healing for others!

Immunohematology Made Easy (2)
General Topics – Key Principles and Everyday Practices
📘 Available now in PDF & EPUB formats
🔗 Visit Store
📘 New to Blood Bank?
Start your 5-day journey with Immunohematology Made Easy — a simple, beginner-friendly guide with real-life examples!
👉 Get Your Copy Now